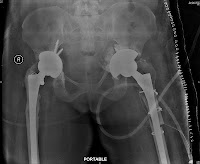
This patient, a 44 year old rheumatoid lady underwent revision of rt hip in 2005 with MOM where in we advised revision of the lt. cup. Financial reasons or otherwise, she comes 7 years later with the cup migration. comments please. Her metal ions are fine. The xrays are in chronological order. Early revision could have saved much bone and made surgery easier.
A collection of complex joint preservation and replacement case studies and random thoughts of a orthopedic surgeon essentially aimed at knowledge dissemination.
Sunday, 15 April 2012
Price one pays for delayed revision in aseptic looseningr
This patient, a 44 year old rheumatoid lady underwent revision of rt hip in 2005 with MOM where in we advised revision of the lt. cup. Financial reasons or otherwise, she comes 7 years later with the cup migration. comments please. Her metal ions are fine. The xrays are in chronological order. Early revision could have saved much bone and made surgery easier.
Monday, 6 February 2012
modified hardinge approach
Modified hardinge Approach maintaing 2/3rds of the medius and releasing towards the lesser trochanter and not vertically downwards maintain the medius- lateralis tension band as well as exposes the acetabulum and the femoral shaft necessarsary for standard THR. Why violate tissue when you dont need to?
Wednesday, 1 February 2012
Revision ACL
5 months after ACL reconstruction Rom 15 to 90. why should this happen. What to do now
On Scopy a "cyclops" lesion was seen. this was shaved of and a wide notch plasty was done to prevent further impingement. Full extension was acheieved however flexion was still limited. The suprapatellar pouch and the medial and lateral gutters were leared of the scar. Patellar mobility and full rom was achieved with medial and lateral patellar release which was the next stage of the plan.
Monday, 19 December 2011
aseptic lossening of cup in a 62 year old female 4 year postop
Why did it fail?
Poor acetabular cementing
Medial wall penentration could cause other problems but not loosening.
Tips for good acetabular cementing
Dont ream the subchondral bone off
The last reamer used should be at least 2 mm or 4 mm more than the cup size to get at least a 2 mm cement mantle with good penetrarion
Don't ream the subchondral bone. Multiple(8 to 10 in no) 4 mm peg holes better than large key holes. Make the key holes wider than the mouth for macro locking.
Dry acetabular bed before cementing
Pressurise after inserting doughy cement
Apply cement on the back of the cup too to avoid blood at the cement implant interface
Insert the cup locking the inferior cement first in an open position before bringing it to 40 degrees and anterverting. Maintain pressure with the head shaped pusher while removing excess cement from the periphery till its hard
Remove any peripheral osteopyhtes to prevent impingement
Finally it is easier to do an uncemented cup well than a cemented cup for the beginner
Do we revise the cup alone?
If we do this, the dislocation chances are higher due to neck cup impingement. To correct this one needs to revise the stem to use a 32 mm or 36 mm head.
How do we revise the stem?
a. ETO and distal fixing uncemented stem
b. Cement on cement revision as advised by Dr. Phil Roberts
We did a cement on cement stem and an uncemented cup without removing the medial cement, obtained could posterior superior contact
Used a high speed drill and stem extraction and cementeda tapered stem with an oxinium on xlpe liner
Sunday, 4 December 2011
52 year old male with aseptic loosening at 3 years
 The patient was advised by the surgeon that the implant was rejected.. This is an example of bad cementing or polywear causing loosening.
The patient was advised by the surgeon that the implant was rejected.. This is an example of bad cementing or polywear causing loosening.
Removal of debri, washing out the blood, dry field are mandatory before cement application. Pressuring, cement gun introduction and timing of implant introduction depends on the type of cement and room temp.
This was definitely not rejected
jacob
Sunday, 20 November 2011
Saturday, 19 November 2011
Knee pain
Sports were designed to improve fitness of ordinary mortals. In our quest for higher level of fitness we sometimes damage joints beyond repair. Some amount of cyclical loading is good for cartilage (the softer shock absorbing ends of bones) nutrition. A Swedish prospective study comparing degenerative wear with exercise compared daily exercise, with thrice daily exercise and no exercise and concluded that thrice daily exercise probably had the least wear.
Once a mechanical change to the alignment or stability of knee occurs, it becomes the beginning of the end of knee. Ligament injuries which contribute to stability are akin to suspension and wheel alignment of our cars. Your continuous driving without correction wears out the tyres similar to the softer cartilage of the knee.
Pain is a protective phenomenon evolved to prevent further damage to oneself and administering of pain killers alone without investigation and treatment of the cause could further deteriorate the joint.. As far diagnosis of cartilage injuries, MRI scans upto 3 Tesla magnets with de-gemmeric software to look at cartilage has improved the diagnosis of cartilage injuries. These days easy reproducible minimal access surgery is available world wide to correct alignment, ligament reconstruction and resurfacing of cartilage injuries using osteoarticular grafts, bioscapholds and matrix assisted autologous implantation.
The use or abuse of exercise is ever increasing in our quest for healthier hearts. Over doing the same has exacerbated the possible incidence of osteoarthritis in knees. Weight reduction is the first simple step to reduce the wear across the cartilage. Six times one’s the body weight goes through our knees while walking. It is akin to driving a truck with cycle tyres. The smaller bony part of the knee has to take the excessive load which is already getting stiffer due to chemical changes and decrease water content with aging. Stronger and fitter muscles do take part of the load.
The role of neutrocaeuticals for arthritis has been controversial. Glucosamine and chondroitin sulphate are normal constituents of articular cartilage, but only 8% gets absorbed and how much reaches the knee is unclear. There are no studies to prove that the cartilage becomes normal with ingestion of neutricaeuticals. It at best could reduce the rate of degradation and might have analgesic effects. There use has been widespread so as to avoid the deleterious side effects of long term use of analgesics which are proven to cause Gastrointestinal and renal problems.
Viscosupplementation have been used to delay the inevitable and recently been talked about as a disease modifying intervention. This is yet to be proved and at best would be a stop gap arrangement till the inevitable knee replacement occurs.
Knee replacement has been shows to be in medium to long term, the best option once end stage arthritis occurs. Newer designs, materials like oxinium and crosslinking of polyethylene have proven to reduce the wear rates and improve the longevity of the implant. The complications of Pulmonary embolism, infection has been decreased with better drugs and early mobilization. As younger arthritic patients are demanding better function newer partial knees are being tested.
Reducing blood loss during joint replacement
Methods to avoid transfusion, more so in bilateral TKR are possibly being achieved by using transxemic acid ,Thrombin, aquamantis and other methods. Our preliminary trial shows a trend towards minimising blood loss in Rheumatoids and bilateral tkrs using FLOSEAL.
Does size matter
The size of the incision or the implant does nothing to the longeivity or function of the implants. It is the technique, quality of bearing, fixation and alignment which is paramount. The approach whether anterior or posterior if done well does not matter. Why are we stuck on the size? yes, it could be a marketing tool. These fads fade away and what matters most is the function and longievity. Smaller Proximal loading stems might have a role in preserving proximal bone. Till date No hip other than resurfacing maitain bone in gruen zone 1 and 6. With the metal on metal controversies surface replacement is used in select cases only.
Wounds heal side to side and possibly better rehab and multimodal analgesis will help to get the patient up quickly.
Thursday, 17 November 2011
migrating stem
protrusio acetabuli in RA

This is 36 year old Doctor with RA on long term steroids. Presented with pain in hip as well as knee.
Why do we wait to complicate reconstruction?
Problems
1. Severe Osteoporosis
2.Huge cavitatory acetabulum with deficient medial and anterior wall
Young patient
Any comments on Options for acetabular reconstruction.
We used a Cone prosthesis and a wagner uncemented cage with ceramic on poly bearing.A peripheral fitting cup was an option but due to the osteopenia, we opted for a cage which came in 2 sizes. I understand Zimmer has withdrawn both these products from Sulzer.
Dislocation in in bipolar of 3 weeks duration

76 year old female presented with dislocated bipolar of 3 weeks duration. she is asa gr 3, memory loss and is a household ambulator. The dislocation occured while sitting on the toilet
The lesser trochanter appears more prominent
Possible causes in general for dislocation
Inadequate Offset
abnormal version and impingement
Options
1. Closed reduction and abductor bracing
2.if found unstable at closed reduction the options
Tuesday, 9 August 2011
Trochlear dysplasia in an 18 year old boy
Subscribe to:
Comments (Atom)